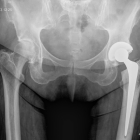
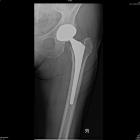
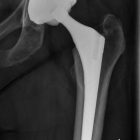
A hip replacement is a surgical procedure performed to treat chronic hip pain usually due to arthritis.
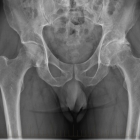
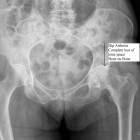
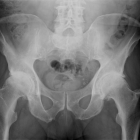
Hip arthritis is a condition where the smooth articular cartilage lining of the hip wears away. Eventually this exposes the underlying bone. Hip arthritis is associated with pain (which may be felt in the buttock, groin, thigh or knee), stiffness and limitation of function.
Hip replacement surgery is a safe and reliable procedure usually resulting in relief of hip pain and stiffness with a return to normal function.
Hip replacement is usually long lasting (20+ years).
Who should have a Hip replacement?
A Hip replacement is usually performed on someone over 60 with arthritis of the hip that is not able to be treated with other therapies. Most patients try medication and or physiotherapy prior to contemplating hip replacement. In patients less than 60 years hip replacement may still be performed if the symptoms are severe enough but there is increased risk.
Before Surgery
Prior to hip replacement most patients will require a medical assessment by a physician. This allows detection and management of medical issues. The physician will also usually be available at the time of the hospitalisation to help manage any medical issues.
Some blood tests will be required.
“Prehab” – Also prior to surgery “prehab” or preparation and exercise prior to surgery make a big difference to recovery. You will usually be seeing a physiotherapist a number of times before surgery to work on range of motion and strengthening. You will also learn how to use walking aids (usually crutches), and advice on hip precautions.
The pre-operative work makes recovering after surgery easier and faster.
The Surgery
Modern hip replacement (minimally invasive surgery) uses much smaller incisions and causes less trauma than in the past although this does depend on the size of the patient.
Minimization of surgical trauma allows for faster and less painful recovery from hip surgery.
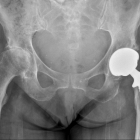
Hip replacement surgery involves removing worn arthritic hip surfaces and replacing them with new implants.
After The Surgery
The most important aspect of hip replacement aftercare for the patient is early safe mobilisation. A physiotherapist will advise you on exercises to do in bed and also assist with beginning to walk again. Mobilisation after a hip replacement requires lots of hard work from the patient. The goals are safe walking, usually with an aid (crutches, walker) and education about hip precautions.
Hip replacements are at risk of dislocation. This means that if the patient attempts certain manoeuvres the hip can pop out (dislocate). The physiotherapists will give you advice on which manoeuvres you need to alter or avoid (hip precautions).
Over time the hip becomes surrounded by scar tissue and the risk of dislocation becomes low. Most patients will achieve the ability to safely walk (with an aid) in a few days. For those who have difficulty a stay in a rehabilitation ward may be appropriate. Patients who prepare well usually have a faster recovery and can avoid the rehabilitation ward. Shorter stays in hospital lead to better results and less risk of complications.
On discharge a physiotherapist will demonstrate how you should get in and out of your car.
Recovery
The recovery time after hip replacement is variable. Some patients have very fast recoveries and others take longer. Most patients will be able to manage crutches and be discharged home from hospital after a few days. Some patients will need longer. By 6 weeks most patients are mobilising well and beginning to return towards normal function, some however will still have pain and stiffness at that time.
Physiotherapy after hip replacement is important. Physiotherapy helps with walking and pain relief and is crucially important with regards to hip precautions.
The Results
Most people do well after hip replacement. There are a number of risks involved with the surgery, these will be explained in detail should you elect to proceed with a hip replacement.
In Australia the National Joint Replacement Registry collects data on all hip replacements performed. Their data shows that after 10 years, 95% of hip replacements are still functioning. This means that 5 in 100 hips will require more surgery in the first 10 years, this usually involves revising the hip replacement to another implant. Reasons for this include infection, failure of implants, dislocation, leg length inequality, pain, etc.
Hip replacement is not appropriate in young patients who wish to perform heavy work.